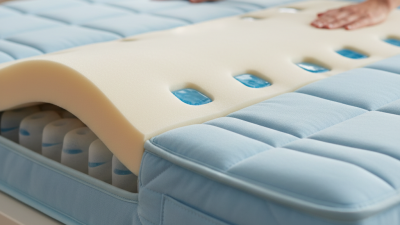
In the world of pressure relief, the "Anti-Decubitus Mattress" emerges as a vital tool. Dr. Emily Carter, a leading expert in pressure ulcer prevention, emphasizes, "The right mattress can make a significant difference in patient comfort and care."
As people spend long hours in bed, preventing pressure sores is crucial. An Anti-Decubitus Mattress helps distribute body weight evenly. This feature reduces pressure on vulnerable areas like the hips and heels. However, not every mattress is perfect. Some users report discomfort or insufficient support, which requires careful consideration.
Choosing the right Anti-Decubitus Mattress is not just about comfort; it's about protection. Look for one that offers adjustable firmness and breathability. Many options exist, but not all are created equal. Take time to assess user reviews and consult with healthcare professionals before making a decision.


Pressure ulcers, commonly known as bedsores, can develop when prolonged pressure inhibits blood flow to the skin. According to the National Pressure Injury Advisory Panel, about 2.5 million patients in the U.S. experience these ulcers annually. Vulnerable individuals, such as those with limited mobility, face the highest risks. When skin gets compressed against bone, it can lead to significant tissue damage.
Anti decubitus mattresses are designed to alleviate pressure and improve blood circulation. These mattresses utilize various materials and designs to distribute body weight more evenly. Research suggests that using these specialized mattresses can reduce the incidence of pressure ulcers by up to 60%. However, selecting the right type can be tricky. Factors like patient weight, skin condition, and mobility levels all play a role in effectiveness.
Some users may find that even with the best mattress, pressure ulcers can still occur. It’s essential to combine the use of anti decubitus mattresses with regular repositioning. Some experts recommend turning patients every two hours. Others believe that simply changing pressure points is sometimes overlooked. Understanding these challenges can help caregivers provide better care.

Anti-decubitus mattresses are designed to provide better pressure relief for individuals at risk of bedsores. Key features include pressure redistribution, which helps distribute weight evenly. This minimizes pressure on bony areas, reducing the risk of skin breakdown.
In addition, look for mattresses with breathable materials. These materials help maintain a comfortable temperature while reducing moisture build-up. A cooler sleeping surface can promote better rest. Consider the mattress's ability to adjust to body contours as well. This adaptability enhances comfort and support, leading to more effective pressure relief.
When choosing a mattress, remember to assess thickness and firmness levels. A thicker mattress often provides more cushioning, while firmness can affect support. It's vital to find the right balance for individual needs. Regularly check the mattress for wear and tear. An old or damaged mattress may not provide adequate relief. Prioritize comfort and functionality to ensure better sleep quality and skin health.
When it comes to pressure relief, using an anti-decubitus mattress can make a significant difference. Studies show that around 60% of patients in extended care facilities develop pressure ulcers. This alarming statistic highlights the importance of effective pressure redistribution techniques. Various methods can enhance the performance of these specialized mattresses.
To maximize pressure relief, proper mattress selection is key. The mattress should evenly distribute body weight. Options such as gel-infused foam and air-filled chambers offer superior support. According to industry reports, using multi-layer foam mattresses can reduce pressure by up to 30%. Regularly repositioning patients can help too. Patients should change positions every two hours to alleviate pressure points.
However, many caregivers overlook the importance of maintaining the mattress. Observations suggest that nearly 25% of mattresses show signs of wear after six months of use. Worn materials can lead to inadequate support. An inspection routine can prevent these issues, ensuring optimal pressure relief. Keeping these practices in mind can help enhance the effectiveness of anti-decubitus mattresses.
When choosing an anti-decubitus mattress, it’s essential to focus on quality. Look for materials that offer a good balance between softness and support. Memory foam is popular for its ability to conform to the body’s shape, but not everyone finds it comfortable. Latex options are also available, providing a firmer feel and good airflow. A mattress that retains heat may not be ideal for long-term use.
Durability is another critical factor. Some mattresses wear down quickly, losing their supportive qualities. Check for warranties that indicate a manufacturer’s confidence in their product. Comfort standards can vary greatly. A mattress may feel perfect during a brief test but could become uncomfortable after hours of use. It’s crucial to try it out in situations that mimic real usage.
Listening to reviews can be helpful but also misleading. Everyone has different needs and preferences. A mattress that suits one person may not work for another. Therefore, reflect on personal comfort and support needs before making a decision. It’s worth investing time in finding a good fit, as comfort greatly affects quality of life.
Using anti-decubitus mattresses can significantly enhance patient comfort and care. These specialized mattresses help distribute body weight evenly. This reduces pressure on vulnerable areas. For staff in care settings, it's essential to regularly assess patients. Not all patients will respond similarly to these mattresses. Some may still experience discomfort or skin issues.
Proper usage is crucial. Ensure these mattresses are set up correctly to maximize their benefits. Regularly check the air pressure if using inflatable types. Training staff on how to monitor and adjust these settings is vital. Take note of any observed changes in patients’ conditions. Communication among caregivers is key. It's easy to overlook minor details, but they matter greatly.
Be vigilant about cleanliness as well. Mattresses should be easy to clean and maintain to prevent infections. Establish a routine for inspecting mattresses for wear and tear. Regular feedback from caregivers and patients can provide valuable insights. This helps in making the necessary adjustments. Consider each patient's unique needs. Flexibility in approach is necessary to achieve the best outcomes.